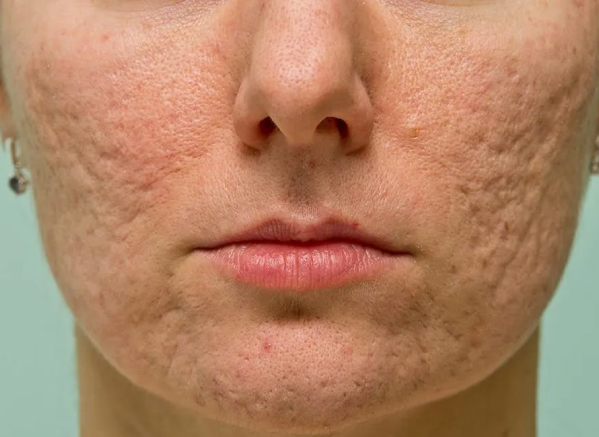
Affects adolescents and adults; managed with topical, oral, hormonal, and procedural therapies.
Overview:
Acne is a chronic inflammatory skin condition of the pilosebaceous unit that commonly presents during adolescence but also affects adults, particularly women. It is the most common skin condition globally and frequently prompts dermatology referral due to its visibility and impact on self-esteem.
Clinical Features:
What Causes it:
Management:
Referral Indications:
Chronic facial erythema, flushing, and sometimes pustules; often referred for persistent or resistant cases.
Overview:
Rosacea is a chronic, relapsing inflammatory facial dermatosis that typically affects adults aged 30–60. It is characterised by facial erythema, telangiectasia, papules, and pustules. Ocular involvement is common.
Subtypes:
Triggers:
Referral Indications:
Common in both children and adults; chronic relapsing course; often referred for moderate-to-severe or treatment-resistant cases.
Overview:
Atopic dermatitis is a chronic, pruritic, inflammatory skin condition with a strong genetic and atopic diathesis. Common in children but can persist into or present in adulthood.
Clinical Features:
Complications:
Management:
Referral Indications:
A chronic inflammatory condition often requiring systemic therapies or phototherapy.
Overview:
Psoriasis is a chronic, immune-mediated inflammatory skin disease affecting 2–4% of the population. It has systemic associations including psoriatic arthritis, metabolic syndrome, and cardiovascular disease.
Clinical Variants:
Common Sites:
Management:
Referral Indications:
Common reasons for dermatology visits, often for reassurance or cosmetic removal.
Overview:
Seborrheic keratoses are benign epidermal growths, commonly seen in middle-aged and older adults. They are often pigmented and have a “stuck-on” appearance.
Clinical Relevance:
Management:
Referral Indications:
Precancerous lesions frequently treated with cryotherapy, topical agents, or field therapies.
Overview:
Actinic keratoses (AKs) are precancerous skin lesions caused by cumulative sun exposure. They may progress to invasive squamous cell carcinoma (SCC).
Presentation:
Management:
Referral Indications:
Often referred for diagnosis, education, and discussion of treatment options.
Overview:
Vitiligo is an acquired depigmenting condition resulting from autoimmune melanocyte destruction. Other common pigmentary disorders include melasma, post-inflammatory hypopigmentation, and pityriasis alba.
Clinical Features:
Management:
Referral Indications:
Increasing presentations, especially with public awareness; often requires specialised management.
Overview:
Hair loss is a frequent cause of dermatology consultation, particularly for distressing or scarring conditions.
Non-scarring types:
Scarring types:
Management:
Referral Indications:
Male and female pattern hair loss is common and frequently causes significant distress.
Common occupational or lifestyle-related skin condition; often investigated with patch testing.
Overview:
Contact dermatitis is inflammation of the skin caused by direct exposure to irritants or allergens. It is common in occupational and domestic settings.
Types:
Diagnosis:
Management:
Referral Indications:
Overview:
Urticaria presents as transient wheals and/or angioedema. Chronic spontaneous urticaria lasts >6 weeks and can severely impact quality of life.
Other itch syndromes:
Management:
Referral Indications:
Includes basal cell carcinoma (BCC), squamous cell carcinoma (SCC) and melanoma; common due to Australia’s high UV exposure.
Australia has among the highest incidence rates globally; dermatologists play a key role in early detection and surveillance.
Overview:
Australia has the highest incidence of skin cancer globally, attributed to high UV exposure and a predominantly fair-skinned population.
Types:
Management:
Referral Indications:
Please refer to the cosmetic dermatology section.
At DVIA, we take the time to listen to your concerns and create a treatment plan that works for your skin, your lifestyle, and your goals. Whether your condition is medical, cosmetic, or a combination of both, our experienced team is here to help.

Book a consultation with a dermatologist at DVIA today.
